- HOME
- News & Events
- Publications
- 【Publications】Pathogen-Induced TLR4-TRIF Innate Immune Signaling in Hematopoietic Stem Cells Promote...
Publications
【Publications】Pathogen-Induced TLR4-TRIF Innate Immune Signaling in Hematopoietic Stem Cells Promotes Proliferation but Reduces Competitive Fitness
July 26 2017
Hitoshi Takizawa
Paper information
Takizawa H*, Fritsch K, Kovtonyuk LV, Saito Y, Yakkala C, Jacobs K, Ahuja AK, Lopes M, Hausmann A, Hardt WD, Gomariz Á, Nombela-Arrieta C, Manz MG* (*corresponding authors)
Pathogen-Induced TLR4-TRIF Innate Immune Signaling in Hematopoietic Stem Cells Promotes Proliferation but Reduces Competitive Fitness.
Cell Stem Cell, 2017, Jul 19. pii: S1934-5909(17)30239-4. doi: 10.1016/j.stem.2017.06.013.
Highlights
- Direct TLR4 activation in HSCs induces HSC cycling and inflammatory responses
- Sustained TLR4 activation in HSCs impairs their competitive repopulating ability
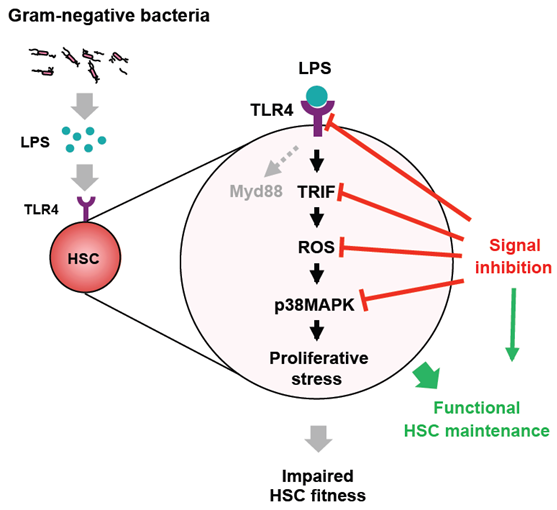
- LPS and S. Typhimurium cause proliferative stress in HSCs via TLR4-TRIF signals
- Inhibition of TLR4-TRIF-ROS-p38 signaling prevents LPS-induced HSC dysfunction
Abstract
Bacterial infection leads to consumption of short-lived innate immune effector cells, which then need to be replenished from hematopoietic stem and progenitor cells (HSPCs). HSPCs express pattern recognition receptors, such as Toll-like receptors (TLRs), and ligation of these receptors induces HSPC mobilization, cytokine production, and myeloid differentiation. The underlying mechanisms involved in pathogen signal transduction in HSCs and the resulting biological consequences remain poorly defined. Here, we show that in vivo lipopolysaccharide (LPS) application induces proliferation of dormant HSCs directly via TLR4 and that sustained LPS exposure impairs HSC self-renewal and competitive repopulation activity. This process is mediated via TLR4-TRIF-ROS-p38, but not MyD88 signaling, and can be inhibited pharmacologically without preventing emergency granulopoiesis. Live Salmonella Typhimurium infection similarly induces proliferative stress in HSCs, in part via TLR4-TRIF signals. Thus, while direct TLR4 activation in HSCs might be beneficial for controlling systemic infection, prolonged TLR4 signaling has detrimental effects and may contribute to inflammation-associated HSPC dysfunction.